Early Detection of Breast Cancer
Why it is so important
Breast cancer is among the most curable of cancers, but the crucial element is early detection. The earlier the cancer is detected, the higher the chances of the patient’s survival.
The 5-year observed survival rate refers to the percentage of patients who live at least 5 years after being diagnosed with cancer. Many of these patients live much longer than 5 years after diagnosis. In order to get 5-year survival rates, doctors have to look at people who were treated at least 5 years ago. Improvements in treatment since then may result in a more favourable outlook for people now being diagnosed with breast cancer.
If detected in the first stage, most patients will survive for more than five years. This figure is 93% when diagnosed in the second stage, 72% in the third stage and 22% in the fourth stage.
If the tumour in the breast remains undetected, the cancer can spread to other parts of the body, like the liver, bones and even the brain. In such cases, the treatment is long and stressful and survival becomes difficult.
Listen to a breast cancer survivor : “I was lucky. I went for my mammogram and my tumour was detected at a very early stage. I didn’t need chemotherapy, my breast was saved and I was in the hospital just for one day.”
Early detection can not only save a patient’s life, it can also help in saving the breast. Moreover, some patients may not require chemotherapy and radiation as part of their treatment in early stages.
Tragically, most women in India pay no heed to the need for early detection. Very few women, even among the educated sections of society, go for screening tests. Women must realise that even if they are in perfectly good health, they must go for screening to eliminate the possibility of a breast tumour. In many cases, if the tumour can be felt as a lump, the cancer had already reached the second stage.
It is important not ot ignore any lump or chenges in the breast- noticed incidentallky or during a breast self examination (video link)
It can happen to anyone
Many women feel that if they have no family history of cancer, they are safe. This is not true. Every day, doctors are diagnosing breast cancer in women with no family history of any form of cancer. Medical science has identified many risk factors for breast cancer (hyperlink to risk factors), but the biggest risk factors are gender and age. To quote one oncologist, “If you are a woman and are over 50 years of age, you are at risk.” What is even more worrying is that younger and younger women are being diagnosed with breast cancer. The reasons are still not clear, though some researchers suspect that the rising incidence of breast cancer could be due to rising levels of chemical pollutants present in the air, water and food.
Even men can develop breast cancer, though the incidence is very rare in men.
Screening for Breast Cancer
Self-examination
This is the simplest technique that a woman can perform, in the privacy of her own bedroom. It is easy, painless and needs no instruments. To learn how to do this, click here (this is either a hyperlink to the You Tube page or the video clip starts on this page itself).
Clinical Examination
A woman’s primary physician or gynaecologist can conduct a full clinical examination to check for tumours or other signs of breast cancer. Each woman should ask her doctor to check her breasts and surrounding areas.
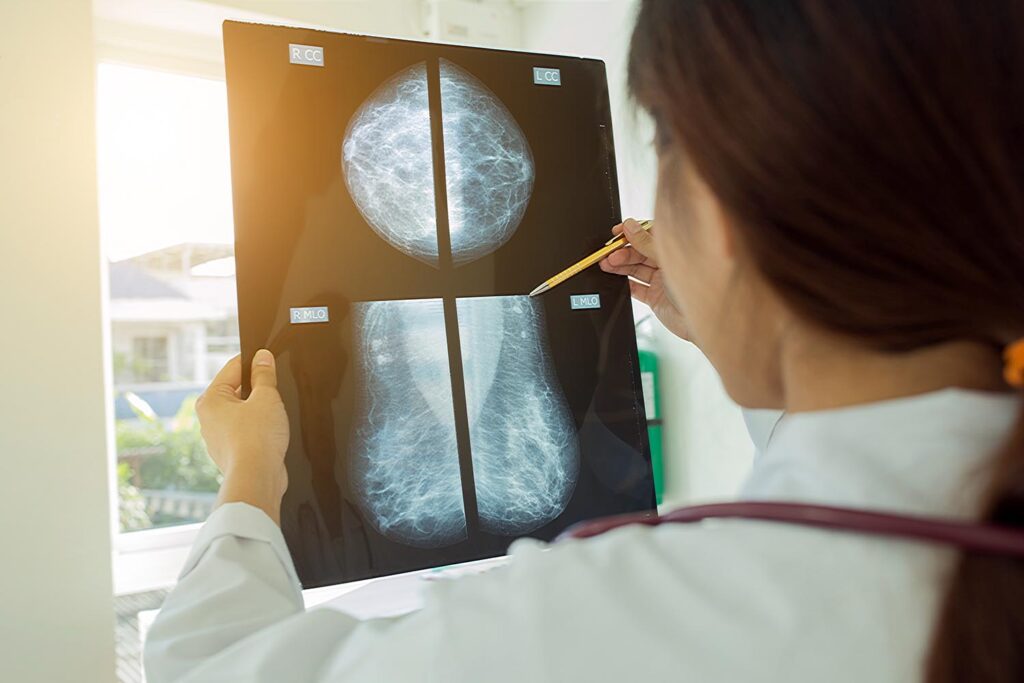
Mammography
This is simply an X-ray of a woman’s breasts, in a machine specially designed for it. A mammogram is still the gold standard for early detection, as it can pick up a tumour much before it can be felt. It also shows a few depositions of calcium, known as micro calcification, which is also an indicator of early breast cancer. But these mammograms must be interpreted only by a trained radiologist.
Ultrasonography
In cases where the breast tissue is dense, especially in younger women, the mammogram may not be able to pick up a lesion or small tumour. In such cases, an ultrasonography would be recommended.
Magnetic Resonance Imaging (MRI)
This is recommended in some instances as a screening tool for women who are at high risk of developing breast cancer. This doesn’t mean that screening mammograms will be replaced by MRI in all women. But your doctor may decide whether an MRI should be done instead of (or in addition to) a mammogram.
High risk factors
- Prior History of Breast Disease – History of breast cancer, regardless of the type, greatly increases an individual’s risk for future development of breast cancer. Such women are strongly advised to carefully monitor themselves and receive mammograms or other investigations on a regular basis
- Family History of Breast Disease – It is possible to inherit defective genes that lead to the development of a familial form of cancer type. Women with a family history of breast cancer are at an increased risk of developing the disease. The degree of risk depends upon the type of relative affected. For example, risk is higher if an immediate family member has been diagnosed with breast cancer. The more closely related an individual is to someone with breast cancer, the more likely they will share the same genes that increased the risk of the affected individual. Risk also increases with the number of relatives affected
- Age – Breast cancer risk is low before age 30 and increases with age, leveling off at the age of 80
- Race – Indian women have a lower risk of developing breast cancer than their American or European counterparts
- Reproductive and Menstrual History – Exposure to estrogen is associated with increased breast cancer risk. For this reason, women who experience menarche (begin their menstrual cycle) before age 12 and the onset of menopause at age 55 or older are at an increased risk of developing breast cancer. On the other hand, women who carry pregnancy to full term at a young age have a decreased risk of developing breast cancer
- Radiation Exposure – Exposure to radiation, such as radiation therapy used to treat Hodgkin lymphoma, increases risk of breast cancer throughout the remainder of a woman’s lifetime. Women irradiated at a young age (before age of 30) are at an increased risk of developing breast cancer later in life compared to older women. Advances in therapeutic radiation techniques have resulted in the use of lower doses of radiation and exposure of smaller regions of the body. Such advances will hopefully reduce breast cancer risk due to irradiation therapy in years to come
- Dietary Factors – It is very difficult to identify dietary items that cause a particular cancer. Factors that may increase breast cancer risk include high fat intake, high alcohol consumption, and a diet rich in overcooked meats
- Drinking Alcohol – Research consistently shows that drinking alcoholic beverages increases a woman’s risk of breast cancer, particularly hormone-receptor-positive breast cancer. Alcohol also may increase breast cancer risk by damaging DNA in cells
Factors that may reduce risk
- Periods starting after the age of 12
- Menopause before the age of 45
- Having children (especially having the first before the age of 20)
- Breastfeeding (for a minimum of five months – this could be one baby or more)
- Risk-reducing surgery (only for those who have inherited a faulty gene)
- Remember one person may have many risk factors and not develop breast cancer, while another may have very few risk factors and be diagnosed with the disease
Fine Needle Aspiration Cytology
- Women should know how their breasts normally look and feel and report any breast change promptly to their doctor. Monthly Breast self-exam (BSE) is an option for women starting in their 20s
- Mammograms starting at age 40 (at least once in 2 years); and yearly starting age 50- and continuing upto the age 75 or as long as a woman is in good health
- Clinical breast exam (CBE) about every 3 years for women in their 20s and 30s and every year for women 40 and over
Signs & Symptoms
A woman should get familiar with the normal look and feel of her breast, nipples and underarm area and then keep a lookout for changes like:
- A lump or thickening of the tissue
- A change in the texture of the skin or an enlargement of the pores, usually known as ‘skin like orange peel’
- Any skin discoloration
- Skin becoming scaly, red, swollen or developing ridges
- Dimpling or puckering anywhere on the breast
- Any unexplained change in the shape and size of the breast
- Any unexplained shrinking or swelling of a breast, especially if it is only on one side
- Change in shape or appearance of the nipple
- Any nipple discharge – clear or with blood
Contact your doctor if you notice these symptoms. It is important to note, however, that these symptoms may be caused by factors unrelated to cancer.

